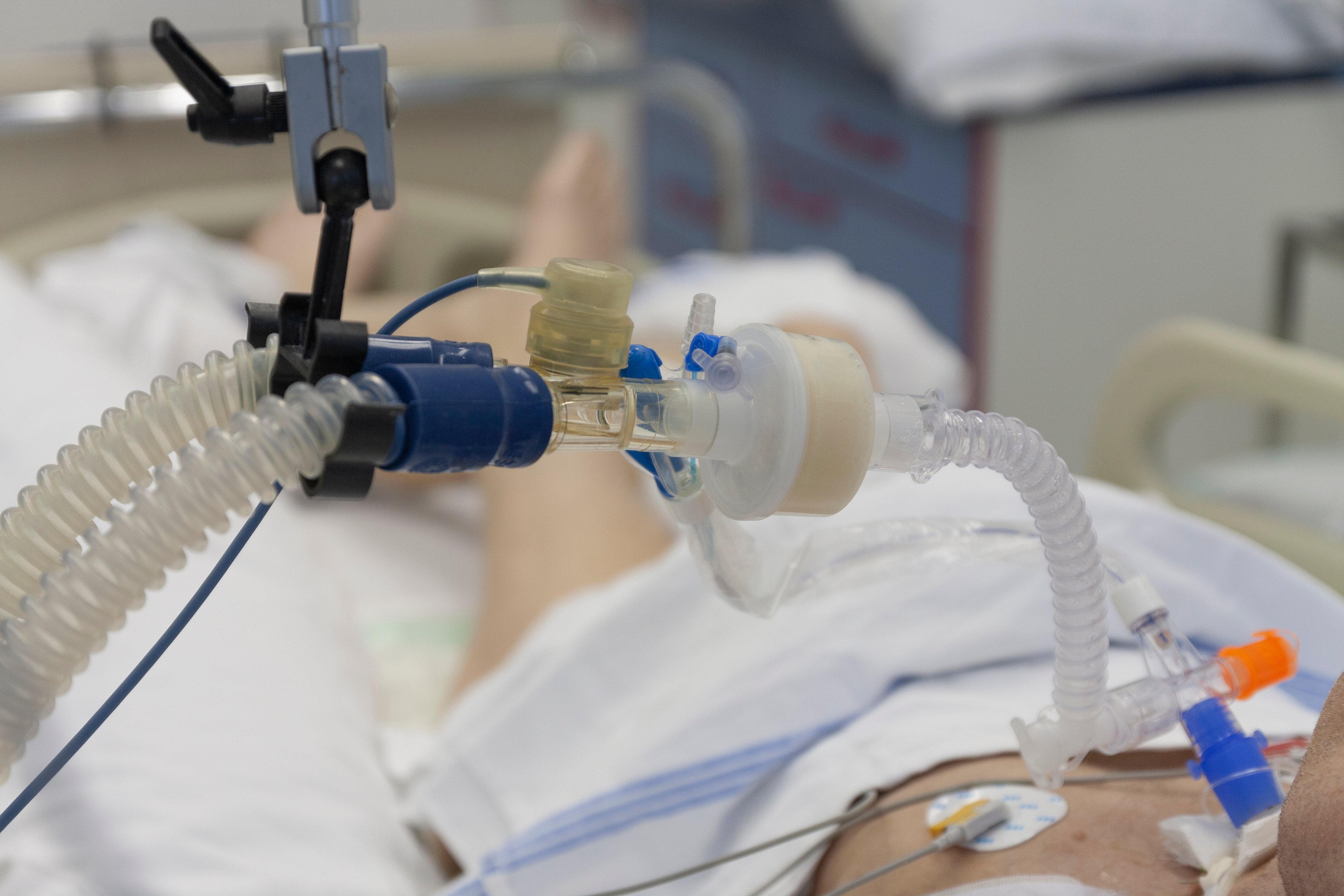
The COVID-19 pandemic has changed virtually everything about medicine. From surgery and childbirth without a support person to delaying routine medical care, the reverberations of the crisis extend well beyond those who become infected. First responders have had to rethink much about their emergency preparedness strategies, particularly now that once-routine procedures present a high risk of disease transmission. Here’s what you need to know about performing tracheostomies during the coronavirus.
COVID-19 and Tracheostomies: The Basics
About 5 percent of patients with COVID become critically ill, with significantly more requiring hospitalization. Some will need mechanical ventilation to survive, raising important questions about safety for medical providers. When medical providers risk infection, they also risk infecting their patients. So a tracheostomy in a COVID patient could increase risk for people throughout the hospital.
Moreover, it’s not just COVID patients medical providers must worry about. People hospitalized for other issues may have COVID, even if they initially test negative. A significant number of people who spread COVID are asymptomatic or presymptomatic. One study found a COVID false-negative test rate of more than one-third, and even the more optimistic studies suggest that several patients out of every 100 will test negative when they are in fact COVID-positive. Consequently, you must assume all patients are infected, and treat every tracheostomy patient as if they are a COVID patient.
Benefits and Risks of Tracheostomy
The primary risk of tracheostomy, as with all invasive medical procedures, is that it increases the risk of COVID-19 transmission. In patients with a known COVID infection, tracheostomy is often performed at a time when the patient is highly infectious, posing a heightened risk to medical professionals and the patients they serve. Some other concerns include:
- Tracheostomy increases the risk of bleeding, which may be especially dangerous given the coagulopathy complications we are beginning to see with COVID.
- Tracheostomy is most beneficial to patients who will otherwise survive COVID. In this regard, it can prevent serious long-term morbidities. However, its benefit as a life-saving tool is unclear.
- Tracheostomy complication rates may be higher in the most severely ill COVID patients.
The benefits, however, may be too great to ignore this procedure. They include:
- Decreased reliance on sedation. This can be critically important for patients who want to talk to and video chat with their families, especially when they may die.
- Less reliance on mechanical ventilation.
- Greater secretion mobility.
- A lower rate of ventilator-associated pneumonia.
- Fewer days on ventilators. This may help free up hospital resources at a time when many hospitals are strained to the breaking point.
Providers must perform a cost-benefit analysis. In some cases, it may be possible to get the benefits of tracheostomy via other means. Diligent suctioning can help remove secretions, for example.
Safe Tracheostomies During the COVID-19 Pandemic
The most important strategies you can use to mitigate risk in tracheostomy patients include:
- Practice diligent, aggressive handwashing after and before touching the patient, touching any equipment, and touching any surface.
- Wear full personal protective equipment (PPE) correctly and to the manufacturer’s specifications.
- Correctly store PPE when not in use so that it is never contaminated.
- Never reuse disposable equipment. Properly store all medical equipment so that it is not in common areas where it might be contaminated.
- Treat all patients as potential COVID patients.
- Never go to work or treat patients when ill, even if the symptoms are minor.
- Talk to your employer about quarantine for COVID patients and those who serve them. A dedicated COVID team who only treats those patients can reduce the spread of the illness to other wings of your facility.
A portable emergency suction machine enables you to treat COVID patients wherever you find them. It also reduces infection spread because it is smaller and portable. That means you do not have to move COVID patients or touch multiple potentially contaminated surfaces trying to access a wall-mounted unit. Seconds matter during a pandemic. For help finding the right device for your agency, download our free guide, The Ultimate Guide to Purchasing a Portable Emergency Suction Device.














