CPR, ACLS, NRP, PAL. As a nurse, you are likely familiar with some, if not all, of these acronyms. Early in your career, you were taught the skills to resuscitate a patient in cardiac or respiratory arrest. Every few years, you attend a class to review and renew your certification.
But is it enough? If your patient suddenly coded, do you feel comfortable with the training you have received? Do you know how to initiate the Code Blue? Do you know where supplies are located in your crash cart? Do you know how to operate your portable suction machine?
What about the other members of your resuscitation team? Can you function as a smooth unit? What if the code occurs overnight when fewer senior staff are present? How you train can make a big difference.
In-situ Simulation Benefits
Research has demonstrated that simulation is the key to successful and ongoing resuscitation training for medical staff. Simulation of different patient scenarios allows providers to practice their skills hands-on, receive real-time feedback, and improve team communication.
In particular, in-situ simulation has shown some real promise. In-situ simulation means “training in place,” where the practice scenario occurs within the normal clinical environment. During these sessions, providers carry out the “resuscitation” on their units, using the supplies and resources that are typically available to them. This allows providers to gain confidence in their competency to deal with these situations, and it helps to identify knowledge gaps or technical issues that need to be addressed.
Practice Makes Perfect
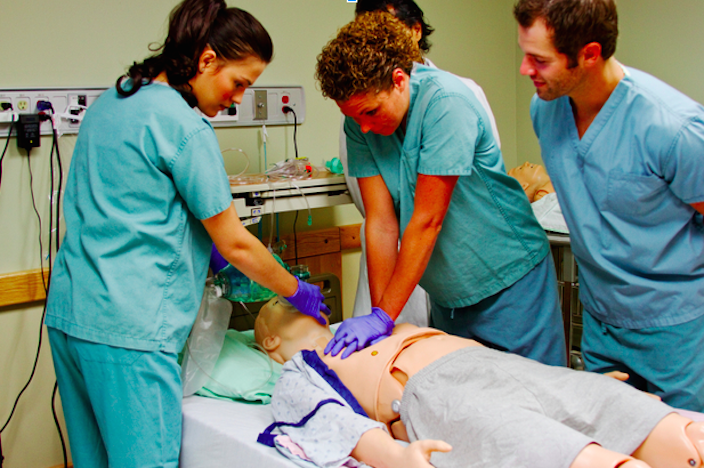
Giving providers an interactive learning opportunity has been shown to increase proficiency in handling high-risk scenarios. Watching a co-worker demonstrate how to use medical equipment or perform a skill will not produce the same level of learning as actually doing it yourself. Setting up a central line procedure tray, manipulating the dials on your portable suction machine, or performing chest compressions – physically performing tasks such as these during simulations will make them easier to implement in a real code situation.
This training improves patient outcomes, demonstrating that hands-on simulations showed a significant improvement in morbidity and/or mortality outcomes following integrated in-situ simulation training.
Continued exposure and practice is the key to safely and effectively managing resuscitations in your hospital. Mock codes and simulation scenarios are an excellent way to identify areas of weakness and gain familiarity with equipment and skills.
Editor's Note: This blog was originally published in October, 2021. It has been re-published with additional up to date content.















