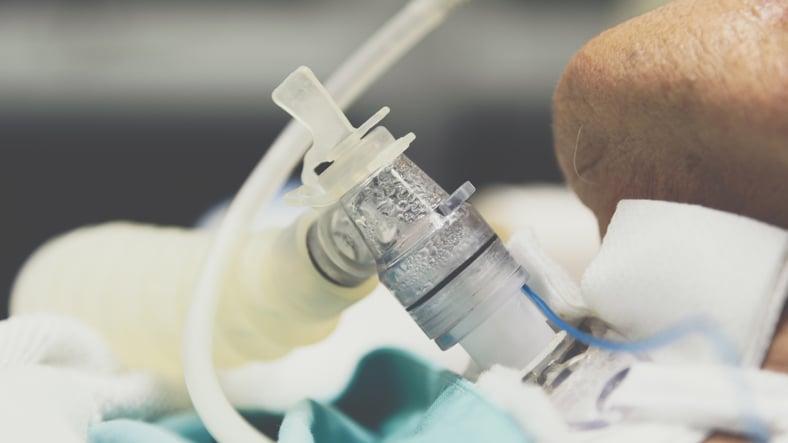
A tracheostomy opens a direct airway into the neck. Its prevalence in long-term care is increasing, and some providers assert that early tracheostomy in mechanically ventilated patients may decrease complications and reduce morbidity.
In the emergency setting, a tracheostomy can save lives when other airway management strategies fail. Like all medical procedures, a tracheostomy presents specific advantages and disadvantages. Here’s what you need to know to make a decision.
Advantages of Tracheostomy
In an emergency, a tracheostomy may be the only option rather than just the best one. In this scenario, the primary advantage of this procedure is that it allows the patient a chance to live.
When there is no other option, first responders should not hesitate to perform an emergency tracheostomy if it is part of agency protocol, because all other considerations pale in comparison to the possibility of dying.
Some advantages of tracheostomy outside of the emergency medicine setting include:
- It may allow a person with chronic breathing difficulties to talk.
- It may eliminate the need for care in an intensive care unit.
- It builds a more stable airway that is less likely to suffer serious injuries.
- It may improve breathing. This may speed healing and improve outcomes in people with chronic, long-term medical conditions.
- It may reduce the need for sedation and eliminate the need for masks and other facial equipment, potentially improving relationships and quality of life.
- It may enable a person who was on a feeding tube to again eat by mouth.
Disadvantages of Tracheostomy
The disadvantages of tracheostomy include:
- Pain and trauma. Tracheostomy can be painful, especially in an emergency setting. Its placement can also be scary. When there is a less intrusive emergency option available, first responders should utilize it.
- Scarring. In patients for whom a tracheostomy is likely to be temporary—including those in emergency settings and people with breathing difficulties that may improve—scarring can be a serious disadvantage.
- Comfort issues. In someone whose length of life is limited, a tracheostomy may improve comfort, or it may be an additional source of trauma. Providers must work with the patient and their caregivers to assess what will be most comfortable in the patient’s final days.
- Complications. A tracheostomy can get infected and cause tracheal bleeding, nerve damage, and erosion of the trachea. Because a tracheostomy bypasses normal infection prevention strategies in the body, the risk of infection is significant.
- Cleaning and additional support. A tracheostomy requires regular cleaning when it is used over the long term. People with tracheostomies may also require more breathing support. This skilled care may limit their living arrangements and compromise their lifestyles.
Tips for Making a Decision
Whether or not to place a tracheostomy should always be a joint decision. The medical provider’s role is to give the patient and/or their caregivers reliable, up-to-date information based on the best medical evidence.
Though the provider can and should make suggestions, the patient is the final decision maker. When there is an emergency, providers may choose to perform a tracheostomy without explicit informed consent. If, however, there is time to discuss the procedure with the patient or their family, first responders must still defer to their wishes. Patients have a right to decline care, particularly invasive procedures such as tracheostomy.
In patients with tracheostomies, regular suctioning is the primary defense against infection and clogging. A quality suction machine allows the patient to remain healthy and comfortable. A portable suction machine can help in the event of an emergency, but may also play a role in daily care depending on where the patient lives and who cares for them. Every agency should have such a machine available. For help choosing the right one for your organization, download our free guide, The Ultimate Guide to Purchasing a Portable Emergency Suction Device.
Editor's Note: This blog was originally published in April 2020. It has been re-published with additional up to date content.
















