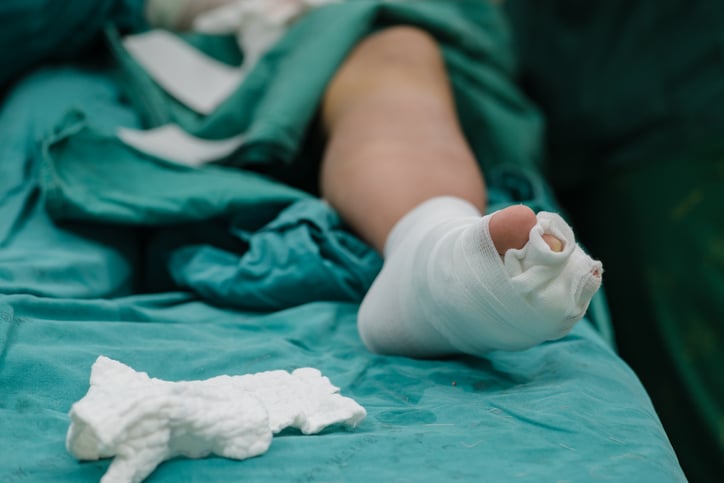
Even minor wounds can be distressing, especially in patients with bleeding disorders or communicable diseases. Major wounds can be life-threatening, necessitating a prompt response that anticipates complications such as bradycardia and shock. Wound management is a cornerstone of good emergency medicine, and so careful planning and frequent preparation should be part of every team’s continuing education.
Control the Spread of Infection
Treat every patient as if they have a communicable disease. First responders should also behave as if they have open wounds that could infect the patient. Wear gloves and, if the wound is spurting, a mask or other protective gear. Thoroughly wash hands before and after tending to the patient, and take proactive measures if you come into contact with blood or other bodily fluids.
Assess and Manage Bleeding
Wound management begins by immediately controlling bleeding, particularly if the wound is deep, and is near a major artery or vein. Direct pressure with a hand is the best strategy for controlling bleeding; tightly applied gauze is no substitute. Tourniquets can help control bleeding over the short term, but are not a safe long-term strategy. Most guides recommend using them only so that you can visualize the wound and temporarily maintain a clean field for administering treatment.
You must also be mindful of the risk of internal bleeding. Car accidents, falls, and other injuries raise the specter of organ injuries. Patients with airway complications may have active bleeding in the mouth or airway. Continuous suction using the suction-assisted laryngoscopy and airway decontamination (SALAD) technique can reduce the risk of aspiration.
Manage Patient Pain
Wounds can be intensely painful. This pain can compromise a patient’s ability to communicate, and intensify other complications, such as changes in heart rate or breathing issues. It’s also completely unnecessary. First responders must take patient pain seriously. So after the bleeding is controlled, work to control the pain. If you must suture or debride the wound, anesthetize the area before proceeding with treatment. If a patient’s pain seems disproportionate to the severity of the injury, consider the possibility that there may be another injury.
Anticipate Additional Complications
Wounds can be distractions, even when they are serious. Sometimes the more serious injury is not so obvious. For example, a patient with a chest or back wound may have also suffered a head or spinal cord injury during a fall. Patients with compromised immune systems may face additional risks, such as the danger of an infected wound that turns septic. It’s important for first responders to conduct a comprehensive patient evaluation to assess for other problems. Perform a respiratory assessment, check the heart, and check for signs of cognitive impairment. Ask about the patient’s recent vaccine and travel history, as well as any long-term or acute illnesses.
Have the Right Equipment Available
Sutures, anesthetics, tourniquets, and equipment such as gloves for minimizing infection are basic tools in every first responder’s toolkit. But in crisis situations, you must be prepared for a wide range of bleeding-related complications. Airway management equipment can help you tend to a patient who suffers a hemorrhage, low blood oxygen secondary to a hemorrhage, cardiac arrest following a traumatic injury, and/or other prevalent complications.
Wounded patients can suffer additional injuries when you move them before they are stable. This is why every organization, including hospitals, must have emergency suction readily available. The right suction machine helps you meet your Emergency Medical Treatment and Active Labor Act (EMTALA) radius requirements, and reduces treatment delays while delivering reliable, consistent suction. For help choosing the perfect suction machine for your agency, download our free guide, The Ultimate Guide to Purchasing a Portable Emergency Suction Device.













