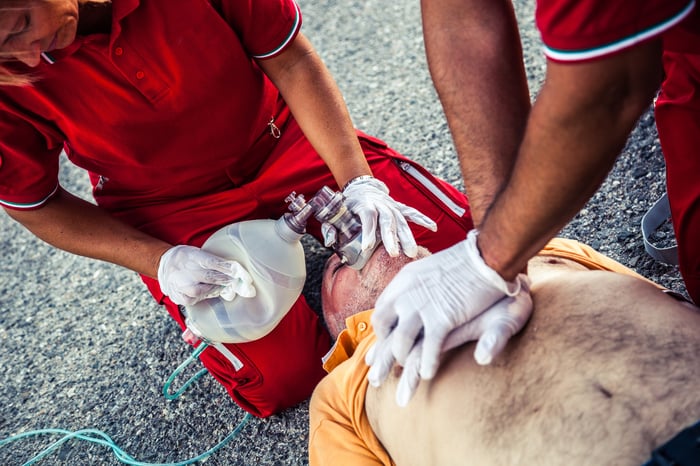
 One of the most critical scenarios a paramedic will respond to is a respiratory emergency. Respiratory distress can be linked to many underlying medical problems, so it must be recognized immediately, treated proficiently, and monitored continuously. But like any medical emergency, treatment begins with a good assessment.
One of the most critical scenarios a paramedic will respond to is a respiratory emergency. Respiratory distress can be linked to many underlying medical problems, so it must be recognized immediately, treated proficiently, and monitored continuously. But like any medical emergency, treatment begins with a good assessment.
So, let’s review the fundamentals of a proper respiratory assessment.
Identifying Respiratory Distress
A patient’s complaint of difficulty breathing is subjective. As with pain, you must rely on what your patient tells you to gauge his or her status. But there are also visible signs of respiratory distress that you must recognize. They include:
- General appearance
- Vital signs
- Respiratory rate
- Pulse
- Oxygen saturation
- Capnography
- Level of consciousness
- Obvious signs of distress
- Positioning
- Anxiety
- Tachycardia
- Tachypnea
- Skin color and moisture
- Diaphoretic?
- Pale or cyanotic?
- Signs of imminent respiratory arrest
- Decreasing level of consciousness
- Patient tiring/exhaustion
- Cyanosis—a late sign and unreliable
How Hard Are They Working to Breathe?
Assessing work of breathing is another vital step in identifying respiratory distress. If your patient is having to work to breathe, something is wrong. Here are five key signs that your patient is working too hard:
- The use of accessory muscles and obvious retractions
- Inability to speak smoothly
- Inability to lie flat
- Diaphoresis
- Agitation and restlessness that will decline to the loss of consciousness
Identify the Pattern
The pattern of breathing can also be a good indicator of an underlying problem, so be sure to observe and document the patient’s respiratory pattern, especially if it changes.
- Kussmaul’s respirations: fast and deep labored breathing, often punctuated by sighs, associated with metabolic acidosis
- Cheyne–Stokes: a cyclical pattern of breathing of progressive increased rate and depth of respirations followed by periods of apnea; often associated with overdose, acidosis, and increased ICP
- Apneustic breathing: prolonged periods of gasping inspiration followed by brief, ineffective expiration
- Hyperventilation: increased rate and depth of respirations associated with anxiety, fever, exertion, acid–base imbalance, or damage to the midbrain.
- Bradypnea: abnormally slow rate of respiration associated with drug or alcohol ingestion, central nervous system lesions (both traumatic and non-traumatic), metabolic disorders, and fatigued patients
- Apnea: the absence of respirations
- Agonal respirations: an abnormal pattern that can be slow, shallow, deep, or gasping
Listen to Your Patient
Lung sounds are critical to a proper respiratory assessment. They can indicate what type of underlying disorder is affecting your patient. They include:
- Wheezes: indicating a constricted airway
- Crackles: also called rales; heard when collapsed airways or alveoli pop open or when there is mucus in the airway
- Rhonchi: associated with mucus in the airway
- Stridor: a “seal bark” often accompanying infection, swelling, trauma, disease, or a foreign body
Treatment begins with assessment, and no emergency is more critical than those involving the respiratory tract. Early identification is key, so stay alert for the signs and symptoms of respiratory distress and always conduct a thorough assessment.
Editor's Note: This blog was originally published in December 2016. It has been re-published with additional up to date content.
















